The short answer is you and me, and most folks we know.

President, American Association of Naturopathic Physicians
“In my opinion, there are two types of people who see naturopathic doctors: those who are proactive about their health and view NDs as an integral part of their healthcare delivery team, and those who see NDs as a last resort, because nothing else has worked for them.”
Without naturopathic patients, there would be no naturopathic doctors. Naturopathic medicine takes a holistic approach to patient care. Therefore, the relationship between the ND and the patient plays a key role in the healing process. An open relationship can help improve a patient’s health, while a closed relationship may be a barrier to recovery. When doctors and patients work together, healing happens.
What patients say they value most about seeing an ND
- They can be active participants in their health creation and wellness.
- Time. NDs typically spend an hour or more with new patients and 30-45 minutes in follow up visits.
- Addressing the root cause, and not focusing solely on symptom management.
- The holistic approach to care that includes nutrition, herbs, supplements and mind-body medicine.
- That their ND takes the time to teach them how to stay well.
- And in the words of many, “I feel heard, for the first time.”
Click here to view a few naturopathic patient success stories.
Common Conditions Treated
Some of the common conditions patients come to see NDs for include gut health, endocrine imbalances, fatigue, anxiety, allergies/autoimmune disorders, insomnia and pain. According to the 2020 AANMC Career Growth and Compensation Survey, approximately 50% of US-based NDs also offer a sliding scale to increase accessibility to various patient populations.
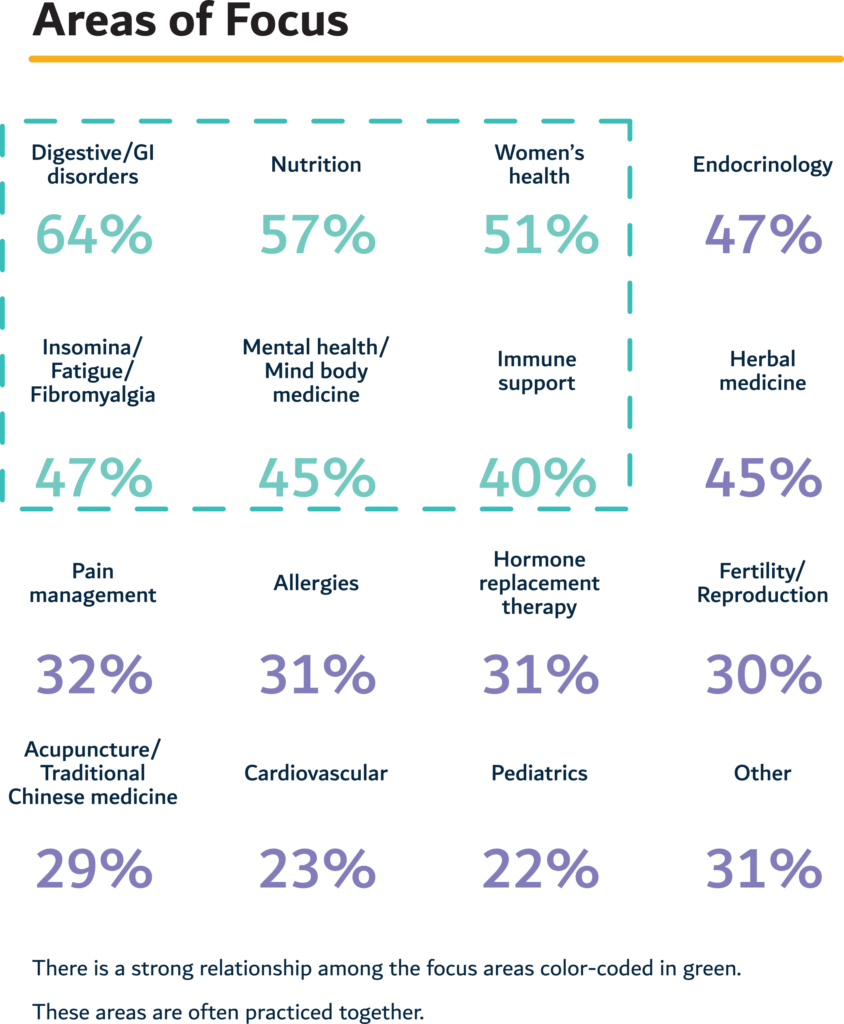
Reference: AANMC Career Growth and Compensation Survey, 2020 *Totals do not equal 100% as many NDs use multiple therapies and approaches to help patients get well.
Naturopathic medical education is extremely comprehensive, and patients may see their ND for primary care, or for a specific area of specialization. NDs treat a wide variety of patients and conditions primarily in outpatient, private and interdisciplinary practice settings.
Naturopathic Specialty Associations exist for the following disciplines:
- American Association of Naturopathic Midwives (AANM)
- Endocrinology Association of Naturopathic Physicians (EndoANP)
- Gastroenterology Association of Naturopathic Physicians (GastroANP)
- Homeopathic Academy of Naturopathic Physicians (HANP)
- Institute of Naturopathic Generative Medicine (INGM)
- Naturopathic Association of Environmental Medicine (NAEM)
- Oncology Association of Naturopathic Physicians (OncANP)
- Pediatric Association of Naturopathic Physicians (PedANP)
- Psychiatric Association of Naturopathic Physicians (PsycANP)
ND practices also afford an eclectic mix of therapeutic options. Additionally, many NDs partner or work in interdisciplinary practices, delivering a team-based approach to patient care. From the table below, you will note a strong emphasis on therapeutic nutrition, as it is often core to addressing so many of the chronic illnesses patients present with.

Reference: AANMC Career Growth and Compensation Survey, 2020
Of those who selected ‘other’ the following graphic describes a bit of what they do.

Lastly, the following chart from the 2020 AANMC Career Growth and Compensation Survey illustrates that ND practices typically spend significant time with patients. Full-time practices see anywhere from 11-100 or more patients per week, however the majority of NDs see fewer than 60 patients per week for full-time, full income practices. Both the doctor and patient report higher satisfaction with their interactions. ND practices seeing lower volumes of patients are typically doctors who choose to work part-time in clinical practice and/or supplement their career with work in academia, research, writing, consulting or the nutraceutical industry.
Patient Success Stories
Naturopathic doctors share success stories of interprofessional patient care.

Graduate, Bastyr University
“I am treating a patient with metastatic breast cancer who has been on a trial drug for about two years. During this time, she has experienced joint pain, severe fatigue, as well as insomnia. We had been attributing her fatigue to treatment side effect, however upon deeper investigation we found that she was hypothyroid, likely due to the variety of treatments she has received. By improving her thyroid function, she has regained significant energy as well as improved sleep. She was also starting to develop elevated liver enzymes due to her treatment and although she has been responding well, there was concern she might not be able to continue. Working together with her medical oncologist, we were able to come up with a plan to stabilize her liver enzymes which has allowed her to continue treatment. Additionally, I provided acupuncture, which has greatly improved her pain level and daily functioning.”

Graduate, Sonoran University of Health Sciences
“As a cancer specialist, I see the benefits of interprofessional healthcare firsthand. I really believe that ‘it takes a village’ when it comes to the treatment of a person with cancer. If a patient only sees one physician, there’s realistically only so much care that they can receive. By involving medical, surgical, radiation, and naturopathic oncologists, the care they receive is more rounded and the patient is well-supported; it’s a team effort to provide the best care possible. I also believe the principle that ‘iron sharpens iron.’ The interactions and experience that I’ve had with my multidisciplinary colleagues over the years has made me a better physician, and enhanced the care that I provide by expanding my own knowledgebase.”

Graduate, National University of Health Sciences
“With hopes of making a full recovery after a work-related back injury, my patient considered the advice of his physical therapist to start exercising and lose weight and was referred to me to help with this lifestyle change. After four months, he lost 84 pounds. This patient has started intermittent fasting with continued weight loss.”

Adjunct Faculty and Graduate, Bastyr University
“One of my favorite stories is of a new mother that was in the care of a midwife at my clinic. During her care, she came to me for management of her thyroid with medication, lifestyle, and nutrition, which was very different than what her prior primary care physician was able to offer. Given the nature of my working relationship with her midwife, we were able to jointly manage her care plan, labs, and follow up. In the course of her pregnancy, she required a TDaP vaccine, which she was then able to walk right upstairs and receive with our team. After her baby was born, she was having lactation difficulties. I was able to step in to help with some botanical lactation support, she was able to see our acupuncturist for milk supply augmentation, and was able to connect with our mental health counselor and psychiatric nurse practitioner to assist with her postpartum anxiety and depression. I was able to work with both her mental health team members to offer nutritional and supplemental support, and to ensure that her treatments were synergistic, not overlapping, and certainly not antagonistic or causing harm. Most importantly, she was able receive all of this care in one place. She came in with her baby and was able to move between appointments seamlessly, with each of us shifting rooms to accommodate her while she breastfed or pumped. While there are so many stories like hers, what we have created in our clinic in terms of interdisciplinary and integrated care that holds families is an incredible experience for us as providers, and for the families that we care for.”

Graduate, University of Bridgeport School of Naturopathic Medicine
“A recent success was the complete remission of an intractable case of psoriasis that presented in the ear canals and genitals and produced chronic and constant itching and irritation that was very distressing to the patient. We employed a team approach including nutrition, allergy identification/avoidance and stress/anxiety management. I am happy to report that the patient’s skin lesions healed within six weeks after treatment began and they are still symptom free to this day!”

Graduate, University of Bridgeport School of Naturopathic Medicine
“I had a patient suffering from mental health concerns which were severely impacting his personal and work life. He wanted only all-natural treatment; however, he was taking medications to keep his mood stable. He had an appointment with his prescribing physician, but told me that he wasn’t going. I strongly advised him that it was in his best interest to go to the appointment, explain his desires to his medical doctor and continue taking the medication as prescribed. For him, naturopathic medicine could only work in conjunction with conventional medicine. With the patient’s consent, I reached out to his psychiatrist and sent him my recommendation plan for this patient’s naturopathic appointment. It was so important in this case to have continuity of care including clear communication with his prescribing physician. We were both concerned for the patient’s well-being. In addition, this patient needed the support of naturopathic medicine combined with allopathic care to achieve his optimal state of mental wellness.”
To become an ND patient, click here to find a naturopathic doctor in the United States or Canada.









